RCM Agentic AI — Autonomous Revenue Cycle Automation
Autonomous AI that handles end-to-end revenue cycle workflows — from patient registration and coding to claims submission and payment posting. AI handles volume so your team handles complexity.
Core Features
Intelligent Workflow Orchestration
Specialized AI collaborates across the revenue cycle, optimized for specific tasks. Domain-driven design ensures the system understands healthcare workflows, not just data patterns.
- Task decomposition & parallel execution
- Agent-to-agent communication
- Domain-driven healthcare models
- Adaptive business rules
Autonomous Denial Prevention
AI agents analyze claim patterns, payer rules, and historical denial data to prevent denials before submission. Proactive issue detection catches problems at the source, not after rejection.
- Pre-submission claim validation
- Payer-specific rule matching
- Historical denial pattern analysis
- Automated correction suggestions
Intelligent Claim Processing
From charge capture through payment posting, AI agents manage the full claim lifecycle. 60% faster processing with consistent accuracy and complete audit trails.
- Automated charge capture
- Clean claim generation
- Remittance processing
- Payment variance detection
Adaptive Learning Engine
The system learns from your organization's specific patterns, payer preferences, and historical outcomes. Performance improves continuously without manual rule updates.
- Organization-specific pattern learning
- Payer behavior modeling
- Outcome-based optimization
- Continuous improvement cycles
RCM Workflow Pipeline
End-to-end automation across every stage of the revenue cycle
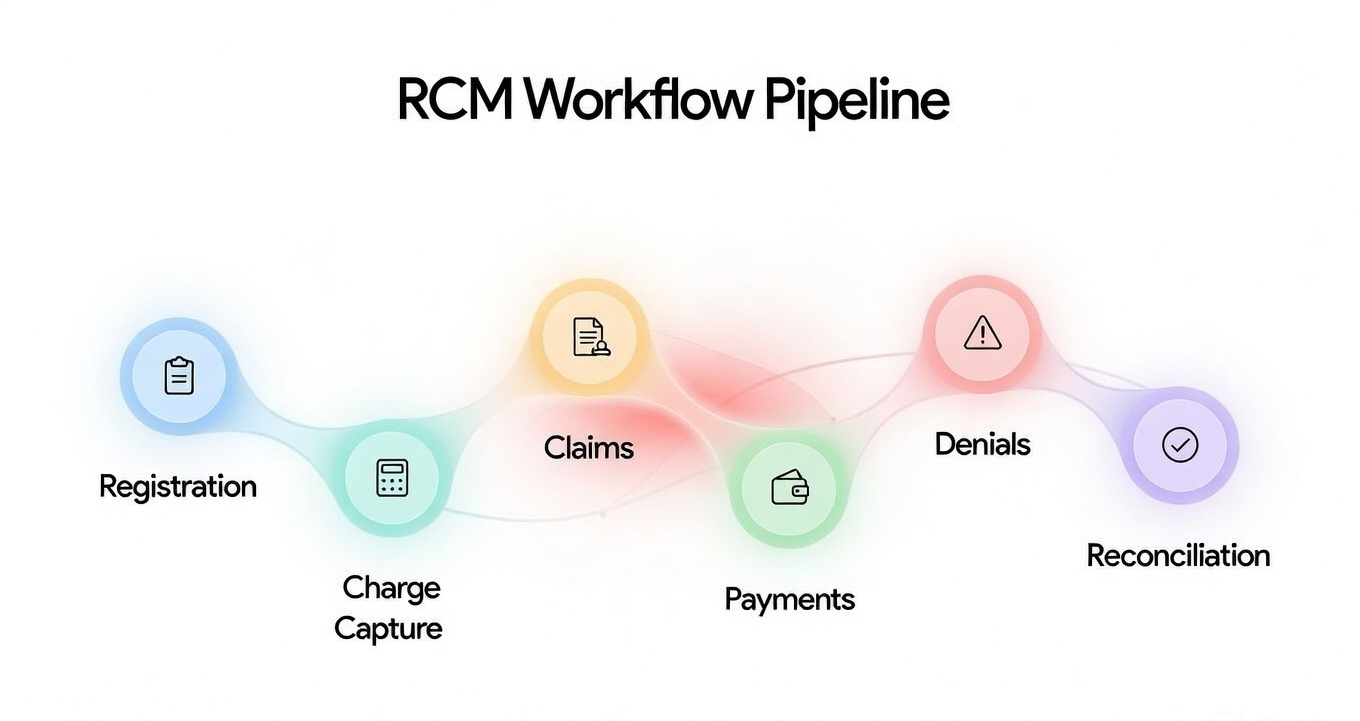
Patient Registration & Eligibility
Automated eligibility verification and benefit checking at point of service
Clinical Documentation & Coding
AI-assisted coding with Anica integration for ICD-10, HCC, CPT, and E/M
Charge Capture & Claim Generation
Automated charge capture with clean claim generation and scrubbing
Claim Submission & Tracking
Electronic submission with real-time tracking and status updates
Denial Management & Appeals
Automated denial categorization, root cause analysis, and appeal generation
Payment Posting & Reconciliation
Automated ERA/EOB processing with payment variance detection